Radiation Therapy for Prostate Cancer
Radiation therapy is a standard curative treatment for prostate cancer. For many years, this required up to 9 weeks of daily radiation treatments due to technological limitations in treatment delivery resulting in large volumes of normal tissue receiving high doses of radiation.

As our ability to target the prostate improved, it became possible to safely deliver higher doses of radiation per treatment. Stereotactic Body Radiation Therapy (SBRT), also known as ultra-hypofractionated radiotherapy, is a curative option for prostate cancer which may be performed in 5 treatments or less.
Radiotherapy has evolved

Prostate motion
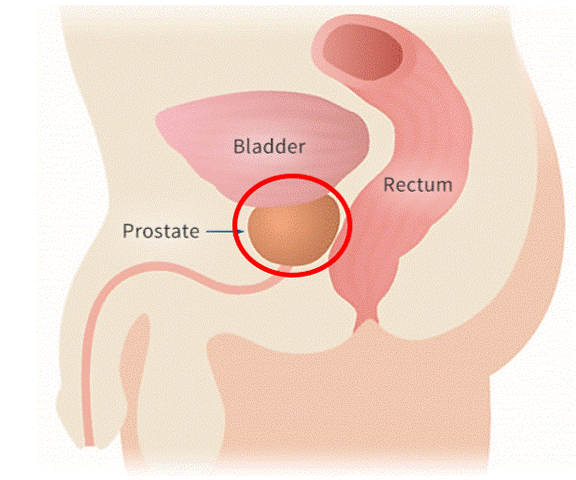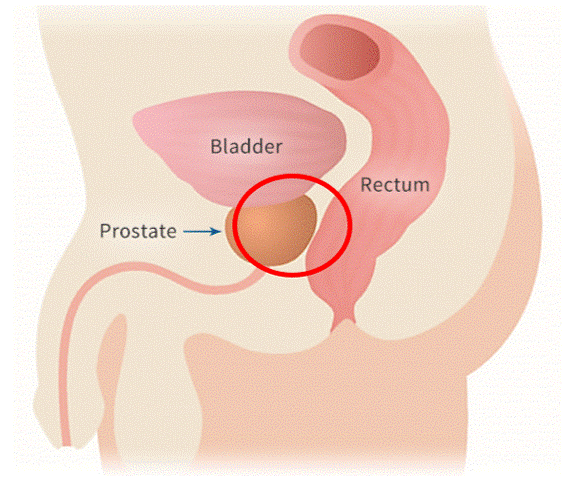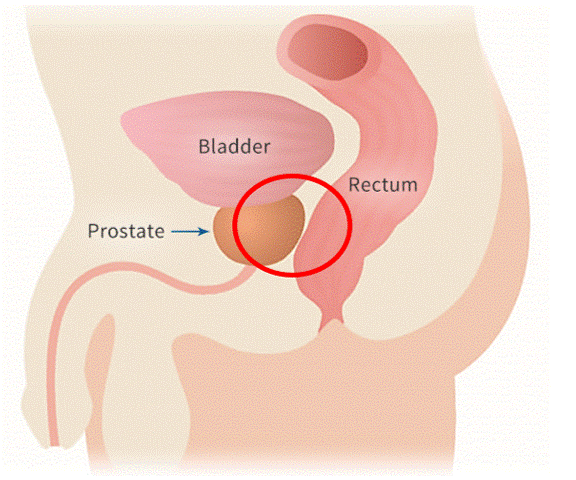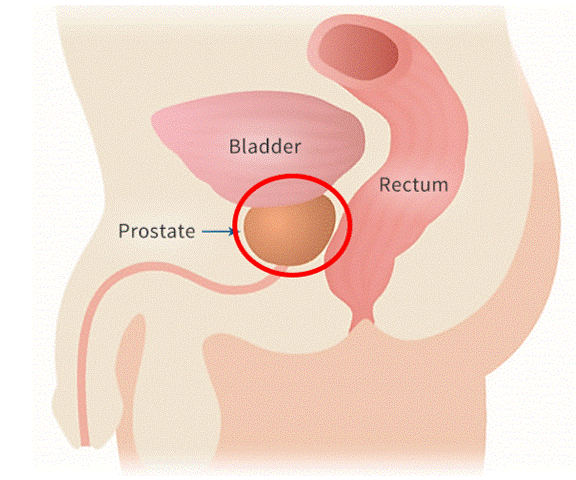
Targeting the prostate
Currently, there are many options available for accurate, real-time localization of the prostate during radiation treatment. One of the original platforms was the Cyberknife, and as such, the name has become synonymous with prostate SBRT.
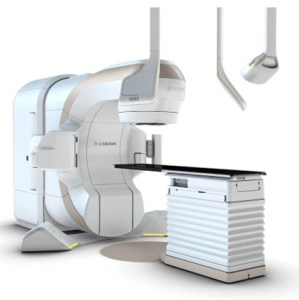
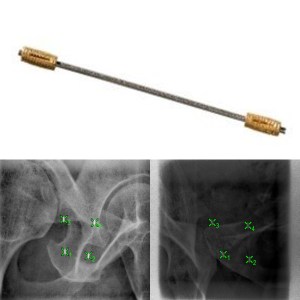


Other platforms include combinations of internal and external imaging such as Varian Advanced Imaging, Brainlab ExacTrac Dynamic, or even real-time MRI imaging as found in the Elekta Unity linear accelerator. Often, small pieces of gold (fiducials) are inserted into the prostate before radiation to help guide the treatment along with a temporary rectal hydrogel spacer. Click below to learn about SpaceOAR.
Prostate SBRT
Who is a candidate for SBRT?
- Any man with organ-confined prostate cancer, and even some with small amounts of cancer outside of the prostate (metastatic) may be eligible for prostate SBRT
- During our visit, we will review all of your medical history and determine which option is best for you and your specific cancer
What is the process for SBRT?
- Initial consultation to review medical history and specifics of your prostate cancer
- If SBRT is right for your prostate cancer and you would like to proceed, you will be scheduled for insertion of prostate fiducials and a temporary rectal spacer. Click here for details
- Following this procedure, you will be scheduled for a treatment simulation where new images of your prostate will be obtained in order to plan the SBRT treatments
- Approximately two weeks later you will begin treatment. There will be 5 treatment sessions spread out over two weeks, each lasting 30 to 60 minutes
What will I feel during treatment?
- Radiation is painless. You will lay on the treatment table and not even realize anything is happening in your body
- As you progress through treatment, you may feel some fatigue, increase in urinary frequency and urgency, increased night time urination, and occasionally discomfort with urination
- These effects are usually temporary and dissipate over 8 to 12 weeks
- Other side effects are mild and you should be able to continue to work or play as usual

Life after treatment
What tests do I need?
Approximately 3 months after completion of treatment, patients resume PSA surveillance. PSA will decline over a period of several years before it reaches its lowest point (nadir).

PSA bounces happen in up to one third of patients and are not indicative of growing cancer in the prostate. The more frequently PSA is checked, the more likely it is to capture fluctuations. I recommend testing no more frequently than every 6 months unless clinically indicated. No other tests are routinely indicated.
Learn more
Watch this explanation by Dr. David Grew, the creator of PRIMR, about PSA monitoring after radiation therapy. You can watch more of Dr. Grew’s prostate cancer explanations by clicking the button below.

